Referring Patients to Salience TMS

Salience Partners with You
Salience sees patients from all across DFW and Houston and at various stages of depression. Our mission is to relentlessly pursue remission and recovery, together, one patient at a time.
We are committed to delivering an exceptional experience to referring physicians and their patients. We respect your ongoing relationships with your patients and appreciate the opportunity to collaborate with you on their TMS Therapy treatment plans.
To refer a patient, you don’t need to know a Salience TMS Therapy Director or have a prior relationship with us. Let us collaborate with you to provide patients with the highest quality TMS care.
Salience has provided more than 500,000 TMS treatments to patients struggling with depression.
Why work with Salience TMS

Patient Success
85% of patients at Salience report seeing improvements in their depression symptoms from TMS Therapy.

Non-Invasive Treatment
TMS requires no sedation, is non-invasive, and lasts only 20 minutes. Patients can drive themselves to and from treatment.

Coordination of Care
Referring Providers will feel connected with the treatment process as we send regular updates regarding your patient. Coordination of care and collaboration is one of our top priorities.

Best-in-Class TMS Therapy
We specialize on one thing: TMS Therapy. This singular focus gives us specialized expertise and training with today’s most effective TMS protocols.
What to Expect when you Refer A Patient

Referring to Salience TMS
It's easy to refer a patient using our online system. Please provide us with some basic demographic information so we can contact the patient, and let your patient know that we will contact them within one business day.
Your patient will receive a call from our Patient Liaison team. Our team will provide them with essential knowledge about TMS therapy, take down their insurance information, and schedule them with a complimentary consult date with one of our patient advocates. We have many locations across DFW and Houston. Our team will work with your patient to schedule them at a location of their choice.

Referring to Salience TMS
It's easy to refer a patient using our online system. Please provide us with some basic demographic information so we can contact the patient, and let your patient know that we will contact them within one business day.
Your patient will receive a call from our Patient Liaison team. Our team will provide them with essential knowledge about TMS therapy, take down their insurance information, and schedule them with a complimentary consult date with one of our patient advocates. We have many locations across DFW and Houston. Our team will work with your patient to schedule them at a location of their choice.
What to Expect During Their Treatment
Before starting treatment, your patient will receive a TMS evaluation from one of our trained TMS Therapy Directors. This TMS evaluation will help to educate your patient on what to expect with treatment and make sure they are a clear candidate for TMS therapy.
It is recommended that your patient receive at least 36 sessions of TMS Therapy. Patients can expect to be in and out in less than 20 minutes for each daily session.
You will receive weekly patient progress updates with PHQ-9 and GAD-7 scores during treatment. In addition, our TMS Therapy Directors oversee treatment, monitor patients' progress, and determine protocol changes based on your patient's response to treatment. They may contact you if they need to collaborate or coordinate with you on their care.
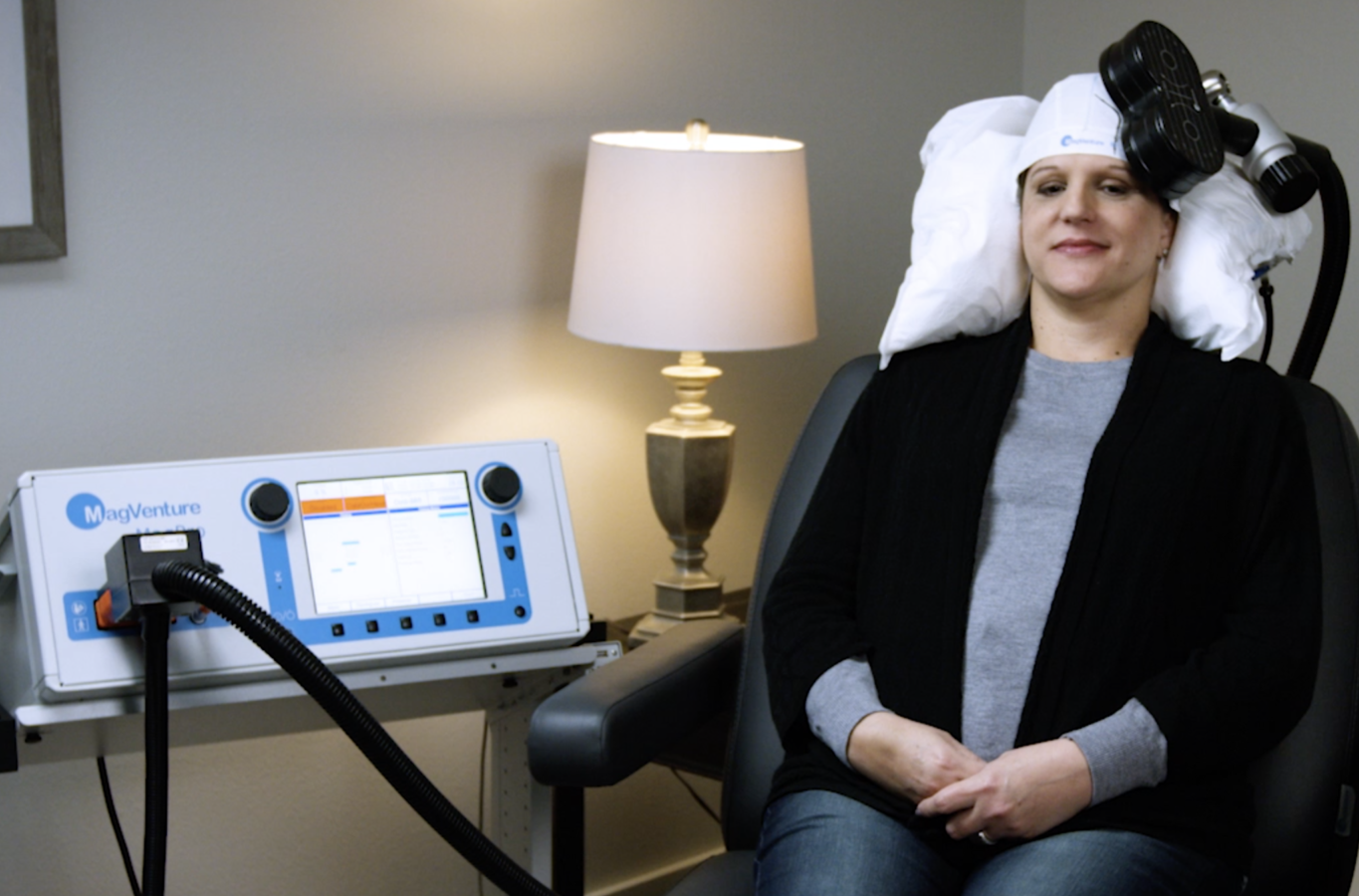

What to Expect During Their Treatment
Before starting treatment, your patient will receive a TMS evaluation from one of our trained TMS Therapy Directors. This TMS evaluation will help to educate your patient on what to expect with treatment and make sure they are a clear candidate for TMS therapy.
It is recommended that your patient receive at least 36 sessions of TMS Therapy. Patients can expect to be in and out in less than 20 minutes for each daily session.
You will receive weekly patient progress updates with PHQ-9 and GAD-7 scores during treatment. In addition, our TMS Therapy Directors oversee treatment, monitor patients' progress, and determine protocol changes based on your patient's response to treatment. They may contact you if they need to collaborate or coordinate with you on their care.

What to Expect Post TMS Therapy
Completing TMS typically takes around 6 to 7 weeks to complete. At the conclusion of the treatment course, you will receive an End of Treatment (EOT) report. The report includes all weekly progress notes, weekly PHQ-9, and GAD-7 scores, and an overall summary of your patient's progress throughout their treatment.
Our team instructs your patients to make a follow-up appointment with you within the next 2-4 weeks. You can also expect your patient's Treatment Coordinator Manager or Patient Advocate to follow up in person and answer any questions you may have about your patient's EOT report.
Finally, your patient will join our Salience Alumni Program which will prompt our team to check in with them regularly to stay proactive on the relapse of their symptoms.

What to Expect Post TMS Therapy
Completing TMS typically takes around 6 to 7 weeks to complete. At the conclusion of the treatment course, you will receive an End of Treatment (EOT) report. The report includes all weekly progress notes, weekly PHQ-9, and GAD-7 scores, and an overall summary of your patient's progress throughout their treatment.
Our team instructs your patients to make a follow-up appointment with you within the next 2-4 weeks. You can also expect your patient's Treatment Coordinator Manager or Patient Advocate to follow up in person and answer any questions you may have about your patient's EOT report.
Finally, your patient will join our Salience Alumni Program which will prompt our team to check in with them regularly to stay proactive on the relapse of their symptoms.
Connect with our Community Awareness Team
What do providers say about working with Salience?

"Salience's comprehensive treatment plan allows the doctor to customize their patient’s treatment and focus on what is only clinically best for the patient. They have added no stress or work to our office and have supplied everything we need to attain results. They are the best structure for TMS Therapy."
Practice Manager, S.P.

